Research and Publications
Research conducted with several populations highlights I-System Interventions’ transdiagnostic efficacy. In studies of veterans, MBB® showed significant improvements by reducing sleep disturbance, symptoms of post-traumatic stress disorder, depression, fatigue, pain, and composite sleep/general co-occurring symptoms, while increasing mindfulness. Furthermore, MBB® has shown to be an effective intervention for the management of insomnia in active-duty military personnel.
A study of cancer survivors showed that MBB® reduced sleep disturbance symptoms as well as symptoms of depression, and improved overall levels of mindfulness, self-compassion and well-being. It attenuated waking salivary α-amylases levels, suggesting positive influences on sympathetic activity in cancer survivors with sleep disturbance, and an increase in oxytocin and in the neuropeptide hormone associated with affiliation, calmness, and well-being in these patients.
A study of individuals suffering from addiction indicated that MBB® significantly reduced drug and alcohol cravings, trauma-related thinking, and disturbed sleep. MBB® also significantly increased mindfulness, self-compassion, and well-being in these individuals. Research with domestic violence offenders indicated that MBB® reduced recidivism and increased treatment compliance. A project conducted with minority communities suggests that MBB® could be an effective tool for achieving improved health among racial and ethnic minority populations.
In a recent publication, Shaun Ho and Yoshi Nakamura present a theoretical and neuroscientific foundation for the I-System Model’s transdiagnostic efficacy. They propose that I-System Interventions like MBB® provide an effective strategy because they address a central problem, such as unrealistic identity-grasping consisting of self-centered embodied expectations, both of self and of others (caused by the I-System), that impairs mind and body well-being.
MBB® has been certified as an evidence-based intervention by the Substance Abuse and Mental Health Services Administration (SAMHSA), an agency within the U.S. Department of Health and Human Services. The Mind-Body Bridging® Substance Abuse Program and the Mind-Body Bridging® Sleep Program have been listed on the National Registry of Evidence-based Programs and Practices (NREPP).
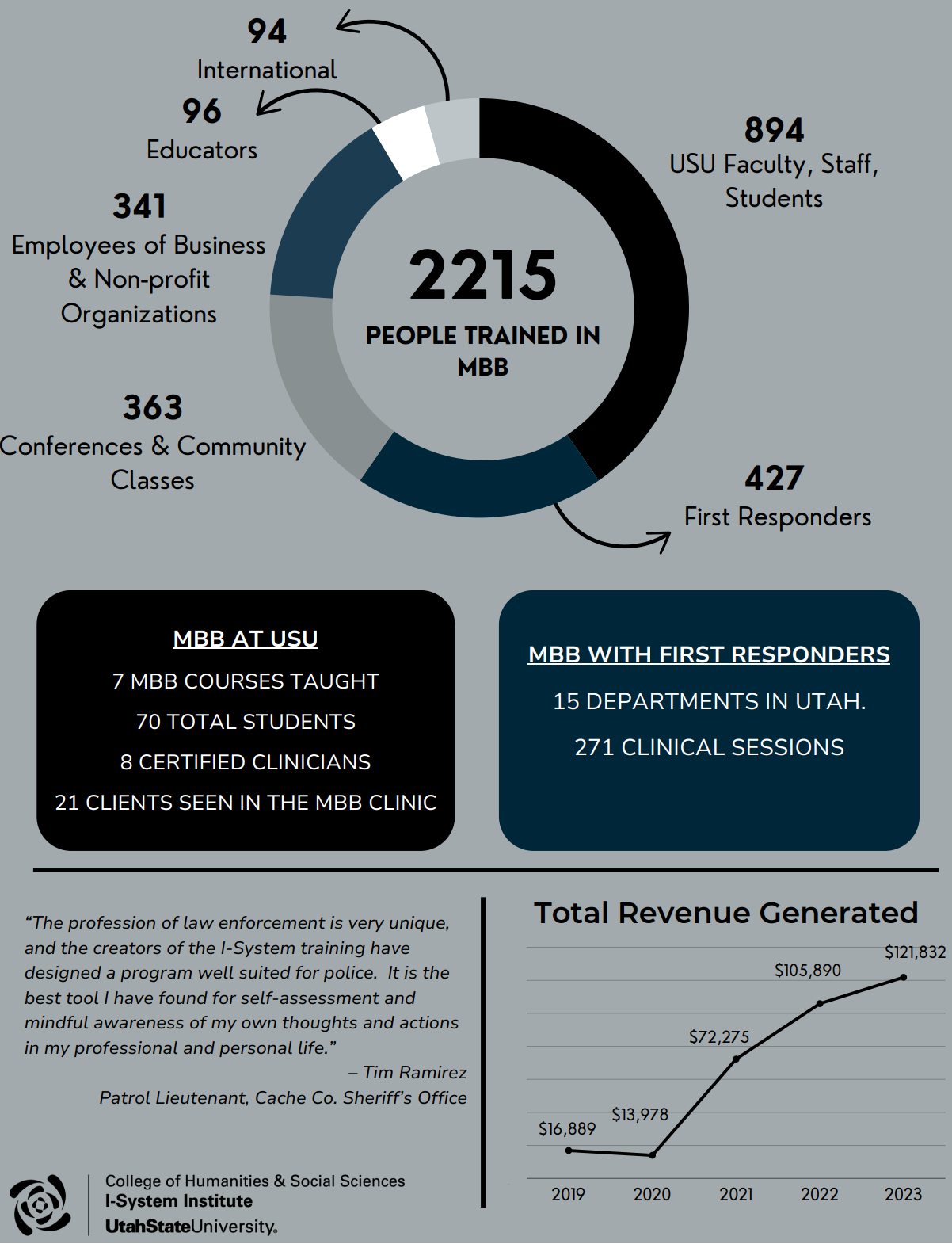
2023 Impact Report

Books
Click on covers to purchase through Amazon.
Recieve a Complementary Copy of Social Unrest

All who donate $20 or more to the I-System Institute for Transdisciplinary Studies will receive a complimentary copy of the Institute's new book, Social Unrest: Resolving the Dichotomies of Me/You and Us/Them by Stanley H. Block, MD and Carolyn Bryant Block, with Derrik Tollefson, PhD & Guy du Plessis, MA.
Building Recovery Resilience Workbook
The first workbook for individuals progressing through the Recovery Resilience Program for addiction recovery and relapse prevention.
Order Workbook
Journal Publications
Audo, Elisa (2012). The experience of mind-body bridging as a treatment for domestic violence offenders. California Institute of Integral Studies, 2012, Dissertation Abstracts International 287; 3508060.
Gren, L. H., Jaggi, R., Landward, R., Benson, L. S., & Frost, C. J. (2016). A Community Health Coach–Delivered Mental Wellness Intervention Using Mind–Body Bridging to Reduce Health Disparities in Diverse Communities. Pedagogy in Health Promotion, 2373379916666299.
Ho, S.S. and Nakamura, Y. (2017) Healing Dysfunctional Identity: Bridging Mind-Body Intervention to Brain Systems. Journal of Behavioral and Brain Science, 7, 137-164.
Lipschitz DL, Kuhn R, Kinney AY, Donaldson GW, Nakamura Y. (2013). Reduction in Salivary α-amylase Levels following a Mind-Body Intervention in Cancer Survivors - an Exploratory Study. Psychoneuroendocrinology. 38(9),1521-31.
Lipschitz, D.L., Kuhn, R., Kinney, A.Y., Grewen, K., Donaldson, G.W., and Nakamura, Y. (2015). An Exploratory Study of the Effects of Mind-Body Interventions Targeting Sleep on Salivary Oxytocin Levels in Cancer Survivors. Integrated Cancer Therapies, 14(4), 366-80.
Lipschitz D.L., Landward R., Nakamura Y. (2014) An exploratory study of an online mind-body program for poor sleepers in a community sample. European Journal of Integrative Medicine, 6 (1) , pp. 48-55.
Lipschitz, D. L., Olin, J. A., Yoshio Nakamura, Y., (2016) A randomized controlled pilot study of a mind-body intervention compared with treatment as usual in the management of insomnia among active duty military personnel. European Journal of Integrative Medicine, 8, (5), 769-780
Lutovac, S., Kaasila, R., Petäjäniemi, M., & Siira, V. (2022). How does mind–body bridging support professional identity development? International Journal for Educational and Vocational Guidance.
Nakamura, Y., Lipschitz, D. L., Donaldson, G. W., Kida, Y., Williams, S. L., Landward, R., ... Tuteja, A. K. (2017). Investigating Clinical Benefits of a Novel Sleep-Focused Mind-Body Program on Gulf War Illness Symptoms: A Randomized Controlled Trial. Psychosomatic Medicine, 79(6), 706-718.
Nakamura, Y., Lipschitz, D. L., Kanarowski, E., McCormick, T., Sutherland, D., & Melow-Murchie, M. (2015). Investigating impacts of incorporating an adjuvant mind-body intervention method into treatment as usual at a community- based substance abuse treatment facility: A pilot randomized controlled study. SAGE Open, 5(1).
Nakamura Y., Lipschitz D. L., Kuhn R., Kinney A. Y., Donaldson G. W. (2013). Investigating efficacy of two brief mind-body intervention programs for managing sleep disturbance in cancer survivors: A pilot randomized controlled trial. Journal of Cancer Survivorship, 7, 165-182.
Nakamura Y., Lipschitz D. L., Landward R., Kuhn R., West, G. (2011). Two sessions of sleep-focused mind-body bridging improve self-reported symptoms of sleep and PTSD in veterans: A pilot randomized controlled trial. Journal of Psychosomatic Research, 70, 335-345.
Tollefson, D. R., & Phillips, I. (2015). A Mind-Body Bridging Treatment Program for Domestic Violence Offenders: Program Overview and Evaluation Results. Journal of Family Violence, 30 (6), 783-794
Tollefson, D. R., Webb, K., Shumway, D., Block, H., and Nakamura, Y. (2009). A Mind-Body Approach to Domestic Violence Perpetrator Treatment: Program Overview and Preliminary Outcomes. Journal of Aggression, Maltreatment, and Trauma, 18 (1), 17-45.
Academic book publications that reference MBB research and MBB programs
Vernon, A. & Doyle (2018). Cognitive behavior therapies: A guidebook for practitioners. Alexandria, VA: John Wiley & Sons, Inc.
Froerer, A., Von Cziffra-Bergs, J., Kim, J. & Connie, E. (Eds.). (2018). Solution-focused brief therapy with clients managing trauma. New York, NY: Oxford University Press.
Lavretsky, H., Sajatovic, M. & Reynolds, C. (Eds.). (2016). Complementary and integrative therapies for mental health and aging. New York, NY: Oxford University Press.
Babson, K. & Feldner, M. (Eds.). (2015). Sleep and affect: Assessment, theory, and clinical implications. London: Academic Press, Elsevier, Inc.
One, J. (Ed). (2019). Cognitive-behavioral therapies for insomnia: An issue of Sleep Medicine Clinics. London: Elsevier, Inc.
Trade books that reference MBB research and MBB programs
Harris, J. S. (2019). Zen beyond Mindfulness: Using Buddhist and Modern Psychology for Transformational Practice. Boston, MA: Shambhala Publications Inc.
Murphy, Christopher M. et al. (2019). Handbook of Interpersonal Violence Across the Lifespan.









